2012 SLICC SLE Criteria
Criteria are cumulative and need not be present concurrently. See notes below.
Clinical Criteria
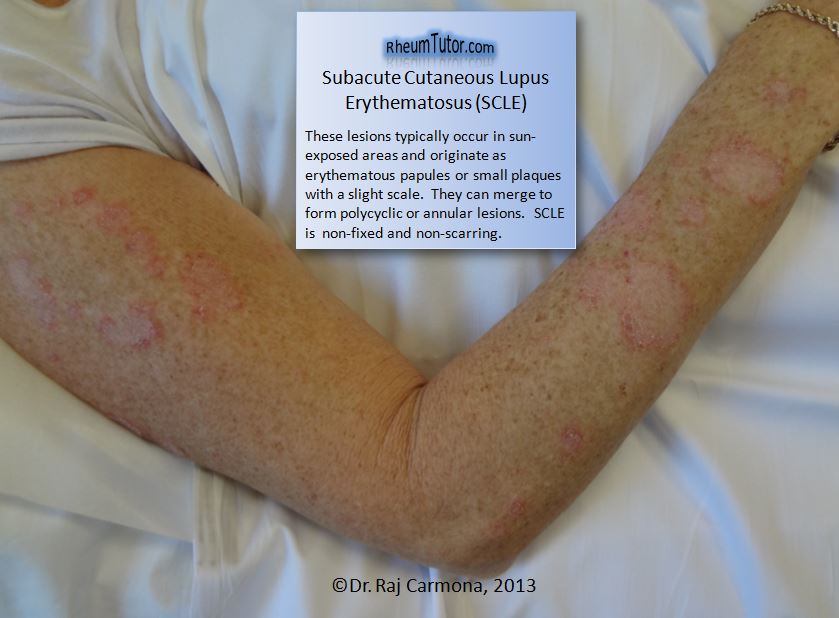
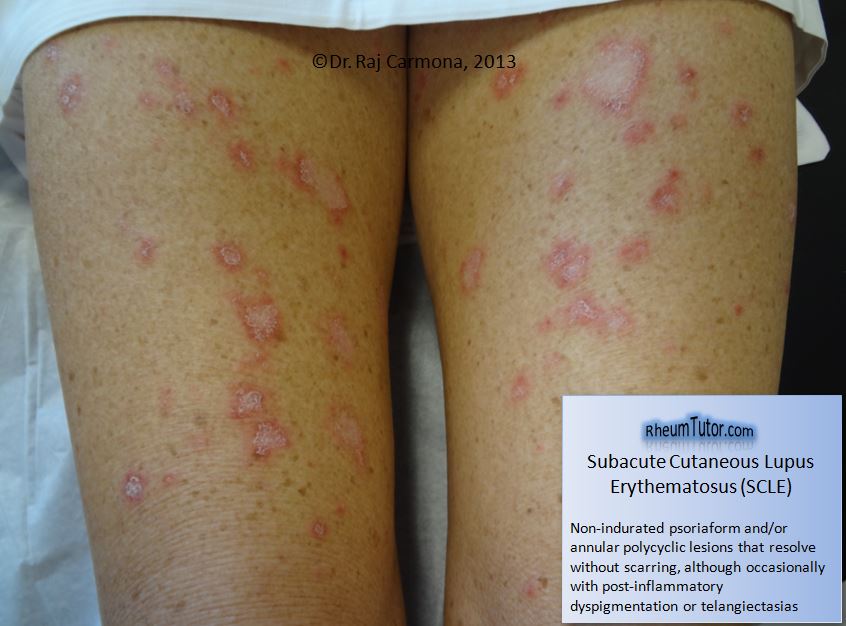
Acute Cutaneous Lupus OR Subacute Cutaneous Lupus
- Acute cutaneous lupus: lupus malar rash (do not count if malar discoid), bullous lupus, toxic epidermal necrolysis variant of SLE, maculopapular lupus rash, photosensitive lupus rash (in the absence of dermatomyositis).
- Subacute cutaneous lupus: nonindurated psoriasiform and/or annular polycyclic lesions that resolve without scarring, although occasionally with postinflammatory dyspigmentation or telangiectasias).
Chronic Cutaneous Lupus
- Classic discoid rash localized (above the neck) or generalized (above and below the neck), hypertrophic (verrucous) lupus, lupus panniculitis (Profundis), mucosal lupus, lupus erythematosus tumidus, chilblains lupus, discoid lupus/lichen planus overlap.
Oral Ulcers OR Nasal Ulcers
- Oral: palate, buccal, tongue
- Nasal ulcers
- In the absence of other causes, such as vasculitis, Behcet’s disease, infection (herpesvirus), inflammatory bowel disease, reactive arthritis, and acidic foods
Non-scarring Alopecia
- Diffuse thinning or hair fragility with visibly broken hairs, in the absence of other causes such as alopecia areata, drugs, iron deficiency, and androgenic alopecia
Synovitis involving 2 or more joints
- Characterized by swelling or effusion
- OR tenderness in 2 or more joints and at least 30 minutes of morning stiffness
Serositis
- Typical pleurisy for more than 1 day OR pleural effusions OR pleural rub
- Typical pericardial pain (pain with recumbency improved by sitting forward) for more than 1 day OR pericardial effusion OR pericardial rub OR pericarditis by electrocardiography
- In the absence of other causes, such as infection, uremia, and Dressler’s pericarditis
Renal
- Urine protein-to-creatinine ratio (or 24-hour urine protein) representing 500 mg protein/24 hours OR red blood cell casts
Neurologic
- Seizures, psychosis, mononeuritis multiplex(in the absence of other known causes such as primary vasculitis), myelitis, peripheral or cranial neuropathy (in the absence of other known causes such as primary vasculitis, infection, and diabetes mellitus), acute confusional state (in the absence of other causes, including toxic/metabolic, uremia, drugs)
Hemolytic Anemia
Leukopenia (<4000/mm3) OR Lymphopenia (<1000/mm3)
- Leucopenia at least once: In the absence of other known causes such as Felty’s syndrome, drugs, and portal hypertension.
- Lymphopenia at least once: in the absence of other known causes such as corticosteroids, drugs, and infection
Thrombocytopenia (<100,000/mm3)
At least once in the absence of other known causes such as drugs, portal hypertension, and thrombotic thrombocytopenic purpura
Immunologic Criteria
- ANA level above laboratory reference range
- Anti-dsDNA antibody level above laboratory reference range (or 2-fold the reference range if tested by ELISA)
- Anti-Sm: the presence of antibody to Sm nuclear antigen
- Antiphospholipid antibody positivity, as determined byPositive test for lupus anticoagulant
The false-positive test result for rapid plasma reagin
Medium- or high-titer anticardiolipin antibody level (IgA, IgG, or IgM)
The positive test result for anti–2-glycoprotein I (IgA, IgG, or IgM) - Low complement (C3, C4, or CH50)
- Direct Coombs’ test (in the absence of hemolytic anemia